Plantar Fasciitis Specialists
Are you an athlete who frequently participates in high-action sports? If so, you may be at an increased risk of experiencing plantar fasciitis. Plantar fasciitis is a common condition of the foot where damage or inflammation occurs to the connective tissue on the bottom of the foot. This can cause debilitating pain, especially after long periods of activity. Complex foot and ankle specialists, Doctors Thomas Haytmanek and Jonathon Backus provide diagnosis and treatment for patients in Vail, Aspen, and the surrounding Denver, Colorado communities who are experiencing symptoms of plantar fasciitis. Contact The Steadman Clinic’s Sports Foot and Ankle team today!

What is Plantar Fasciitis?
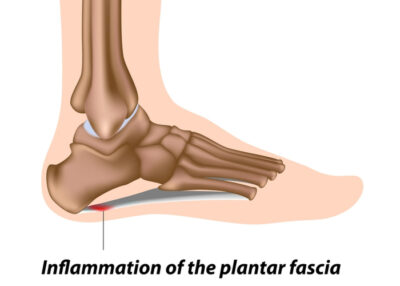
The Plantar fascia is a thick band of connective tissue that runs from the heel to the forefoot. Inflammation of this structure is a common and debilitating condition affects many people each year. This condition is common in athletes and active individuals due to the stress placed on the foot. The cause of this condition can happen for multiple reasons including improper shoe wear with little support, change in shoe wear, change in level of activity, improper training and many times for unknown reasons.
What are the Symptoms of Plantar Fasciitis?
Individuals who have plantar fasciitis will often feel an aching and sharp, stabbing pain in the heel and bottom of the foot. This is often felt with activity and the first few steps when getting out of bed. This can sometimes improve as the fascia warms up with activity. In some patients the pain will again get worse late in the day or with prolonged standing.
How is Plantar Fasciitis Diagnosed?
Our physicians will perform a complete history and examination of the foot including an x-ray. Often times, patients have a bone spur above the plantar fascia. This bone spur has been proven not to be the source of pain in patients, but rather a downstream effect of inflammation at the plantar fascia origin. X-rays will help identify if any other pathology is present as well as the structure of the foot. In some cases advanced imaging (MRI or CT) may be ordered to further evaluate the plantar fascia and other structures.
Does Plantar Fasciitis Require Surgery?
In almost all patients with plantar fasciitis, conservative medical approaches are successful in healing the injury. Generally, non-surgical treatments will be attempted for 6 months to one year prior to consideration of surgical treatment. Treatment includes rest, immobilization (cast or boot), anti-inflammatory medication (both oral and sometimes topical), cushioned heel cups, night splints/boot, stretching and physical therapy. Most often we see patients who have tried one or two of these options. Our experience is that multiple treatments at the same time must be used to get results. We typically recommend use of a night splint, silicone heel cups, and plantar fascia specific stretching three times a day. With these three modalities the pain often subsides over a few weeks to months.
Further treatment if those have failed can include steroid injection, platelet rich plasma injection (PRP), bone marrow aspirate injection (BMCC) or shockwave therapy. The injections attempt to reduce the inflammation and provide additional healing agents to the area. Shockwave therapy is a high intensity ultrasound that can help to stimulate healing but is harder to find providers able to perform this treatment due to insurance restrictions.
What are the Surgical Treatment Options for Plantar Fasciitis?
There are typically two options for surgical treatment of plantar fasciitis. The first option is a minimally invasive removal of the damaged tissue through a small incision on the inside of the foot. A needle is then placed in the diseased area of the plantar fascia and the needle pistons back and forth, cutting and removing the problematic tissue. The procedure is preformed with ultrasound guidance to visualize the diseased tissue and place the needle in an appropriate position. The device used is made by Tenex Health. The procedure involves light sedation and is done in a surgery center. Patients can typically walk the same day in a protective boot.
The second less performed surgical option is release of the plantar fascia. This is performed trough a small incision on the medial foot—releasing half of the diseased plantar fascia. Following this the plantar fascia will heal in a slightly lengthen position. This allows the body to create a fresh healing response as well as decreasing the stress on the plantar fascia. Patient may need a short course of non-weight bearing following this procedure.
What is the Recovery Following Plantar Fasciitis Surgery?
It is essential that patients follow the post-operative protocol for recovery as set forth by our team as it remains a crucial part of the healing process. Depending on the exact surgery performed, patients may resume normal activities within 6-8 weeks. Some patients will require longer recovery if there are concomitant procedures done or the problem was particularly severe.